
 Positive social connections are known to improve human health, so might this be true for dogs as well? Like us, dogs experience the same surge of stress-reducing oxytocin during canine-human interactions.
Positive social connections are known to improve human health, so might this be true for dogs as well? Like us, dogs experience the same surge of stress-reducing oxytocin during canine-human interactions.
The desire to lavish sick or injured canine companions with love and support, without compromising the recovery process, is what led to the creation of ReCover DogCover—a disposable stress-free garment that protects healing areas while allowing dogs to maintain their mobility, confidence, and independence.
What is the ReCover DogCover?
When Duke II, a happy and playful dog owned and loved by ReCover’s founder, was diagnosed with cancer, his life changed. The skin beneath Duke II’s once luxurious coat developed painful sores, creating a heartbreaking barrier between him and the gentle snuggles and loving caresses that once punctuated his daily life. Despite trying every commercially available product as well as DIY options for dressing Duke II, there was simply no way to simultaneously keep him clean and comfortable while maintaining his physical freedom and ability to enjoy an affectionate touch.
Duke II’s owner noticed a dip in Duke’s spirits, as well as her own. Then, in a conversation with her dog’s veterinary oncologist, inspiration struck—and the ReCover DogCover was born.
A different breed of healing: DogCover benefits
Unlike other pet bodysuits, the ReCover DogCover is a completely disposable step-in garment designed to protect healing areas from bites, scratches, and other physical irritants. The DogCover’s material is entirely breathable, creating positive airflow to the pet’s skin and supporting natural thermoregulation to keep pets comfortable. Additional benefits to the DogCover include the following:
- Step-in, suit-up design — No tugging, pulling, or pinching! The DogCover can be placed with the dog in a standing position—simply put their paws in the leg holes and prepare to suit up.
- Custom fit — The full-stretch tear-away fabric ensures a completely personalized fit for every dog, including a tearable perforation along the underside so males can freely urinate without soiling the fabric.
- All day and night wearability — The DogCover’s customizable fit ensures you won’t have to remove the suit for bathroom breaks. The dog stays clean and dry.
- Flexible, full-stretch material — Whether a dog is on post-surgical crate rest or is allowed to run and play, the DogCover’s soft, stretchy material ensures full-body comfort and coverage.
- Antibacterial surfaces — Bacteria-resistant inner layers protect wounds and incisions from irritation and secondary infections.
- Water-repellent outer layer, internal absorbency — The DogCover protects the pup from the elements (e.g., rain, puddles), while the moisture-wicking interior draws natural fluids away from the pet’s wound or incision—ensuring a clean and dry environment.
- UV-resistant, flame-retardant material — All DogCover materials are thoughtfully selected to ensure the dog’s safety.
- Disposable and biodegradable — Don’t worry about disinfecting the DogCover. To ensure the desired hygiene level, each garment is designed for a single use. And because we’re equally passionate about environmental responsibility, the DogCover is 35 percent biodegradable.
In addition to its at-home applications, the DogCover’s convenient, stress-free design and consistent benefits have made it an asset in veterinary clinical settings, including the highly-regarded Animal Medical Center in New York City, where it is being used with great success.
Dressed for success: Reducing post-surgical stress with the DogCover
In addition to protecting your patients physically, the ReCover DogCover enhances their emotional wellbeing by reducing stressors typically associated with the recovery process, allowing them to live a more normal life. Some positive impacts:
- Enhanced comfort — DogCover’s soft, flexible fabric and personalized fit are non-irritating, ensuring the pet can enjoy restful sleep—a critical aspect of healing.
- Fewer changes to the dog’s daily routine — Dogs thrive on consistency and the ability to predict what happens next. By minimizing potentially stressful changes (e.g., putting on and removing a bandage, wrap, or other recovery device, and limiting specific physical activities or interactions), dogs feel more relaxed and confident.
- Inclusion in household activities — Dogs can perform all their normal behaviors while wearing the DogCover, including elimination, eating, drinking, sleeping, going for walks, playing with toys, and simply being part of the family.
- Optimal healing and recovery — Recovery complications can delay your patient’s healing and their return to normal, resulting in additional pain, medications, confinement, and stress. The 24/7 protection provided by the DogCover increases the likelihood of a smooth and timely recovery.
- Uninterrupted affection — When you don’t have to worry about disrupting your patient’s healing or contaminating their incision, you can feel free to spoil them with affection. These positive interactions provide powerful reassurance and can help your patient feel at ease—even when everything else seems out of sorts.
With the ReCover DogCover premium post-surgical recovery suit for dogs, your patients can experience an enhanced recovery journey with less fear, anxiety, and stress, while you can feel confident and empowered to appropriately manage their care.
This article was reviewed/edited by board-certified veterinary behaviorist Dr. Kenneth Martin and/or veterinary technician specialist in behavior Debbie Martin, LVT.
Jaime Bast RVT, CCRP, KPA-CTP, FFCP is a copywriter and registered veterinary technician from St. Louis, Missouri. In her free time, Jaime loves learning about canine nutrition, behavior, and training and competing with her American cocker spaniels in a variety of dog sports.
Want to learn more about Fear Free? Sign up for our newsletter to stay in the loop on upcoming events, specials, courses, and more by clicking here.
Brought to you by our friends at ReCover.



 Brought to you by our friends at Zoetis. ©2022 Zoetis Services LLC. All rights reserved. NA-03139
Brought to you by our friends at Zoetis. ©2022 Zoetis Services LLC. All rights reserved. NA-03139



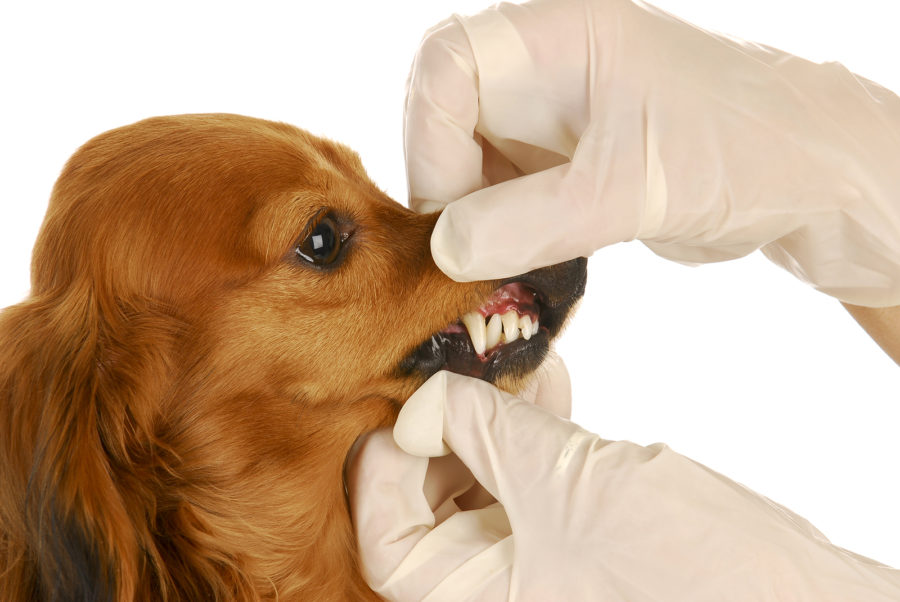
 the mucosa, and the inner surfaces of the lips. Because it’s so painful, a dog may have difficulty eating and be reluctant to open the mouth. This can result in weight loss. Other typical signs include fetid breath, thick, ropey saliva, blood-tinged saliva, visible irritability, depression and lethargy, and pawing at the mouth.
the mucosa, and the inner surfaces of the lips. Because it’s so painful, a dog may have difficulty eating and be reluctant to open the mouth. This can result in weight loss. Other typical signs include fetid breath, thick, ropey saliva, blood-tinged saliva, visible irritability, depression and lethargy, and pawing at the mouth.