
Nail trims are the bane of numerous pets and people. Owners don’t like doing them, and assistants and technicians don’t enjoy being “the bad guys” who have to do the dirty deed. Blood draws and even simple exams can bring bad feelings to the forefront, too. Fear Free to the rescue! Get inspired by fellow Fear Free Certified Professionals as they help pets stay cool, calm, and collected during care.
All About Eva
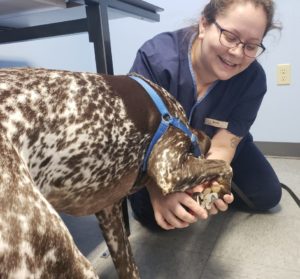 Eva, a spunky and energetic German Shorthaired Pointer, is a staff favorite for more than just her adorable, tongue-hanging-out smile, but there’s one thing Eva never liked: nail trims! Prior to the hospital’s transition to Fear Free in early 2017, it was a challenge to trim Eva’s nails, requiring three or four technicians to assist with restraint, plus a muzzle and calming cap. We started implementing Fear Free teachings right away with all of our patients, but one staff member has really gone above and beyond her commitment to Fear Free training to help Eva overcome her fear. Kayla McNeely volunteered to assist with Eva’s nail trims, and she can now perform Eva’s nail trims solo, standing, with minimal assistance from Eva’s mom, Sheila, who says, “Kayla’s patience and kindness have worked wonders with my girl.” Our hospital requires all staff members to go through Fear Free training to help ensure that all of our clients, patients, and staff have a pleasant experience during their exams. We have seen a tremendous difference in many patients at our hospital since our transition to Fear Free, but Kayla and Eva’s journey together is by far our most successful Fear Free adventure to date.
Eva, a spunky and energetic German Shorthaired Pointer, is a staff favorite for more than just her adorable, tongue-hanging-out smile, but there’s one thing Eva never liked: nail trims! Prior to the hospital’s transition to Fear Free in early 2017, it was a challenge to trim Eva’s nails, requiring three or four technicians to assist with restraint, plus a muzzle and calming cap. We started implementing Fear Free teachings right away with all of our patients, but one staff member has really gone above and beyond her commitment to Fear Free training to help Eva overcome her fear. Kayla McNeely volunteered to assist with Eva’s nail trims, and she can now perform Eva’s nail trims solo, standing, with minimal assistance from Eva’s mom, Sheila, who says, “Kayla’s patience and kindness have worked wonders with my girl.” Our hospital requires all staff members to go through Fear Free training to help ensure that all of our clients, patients, and staff have a pleasant experience during their exams. We have seen a tremendous difference in many patients at our hospital since our transition to Fear Free, but Kayla and Eva’s journey together is by far our most successful Fear Free adventure to date.
Beth Chinnick, CVT and practice manager, Compassion Animal Hospital, East Berlin, Pennsylvania
Ruba Loves Laps
 One-year-old Ruba disliked having her feet touched and her nails trimmed. We trialed trazodone for six months for all nail trim visits. It started to work well, and we discovered she preferred sitting in Dr. DaCosta’s lap. Ruba now comes in for frequent nail trims with minimal restraint and no trazodone needed. We are so proud of her progress and the team’s dedication to using Fear Free techniques.
One-year-old Ruba disliked having her feet touched and her nails trimmed. We trialed trazodone for six months for all nail trim visits. It started to work well, and we discovered she preferred sitting in Dr. DaCosta’s lap. Ruba now comes in for frequent nail trims with minimal restraint and no trazodone needed. We are so proud of her progress and the team’s dedication to using Fear Free techniques.
Brianna King, Clinic Manager, Watzin Veterinary Clinic, Waterdown, Ontario, Canada
Practice Makes Perfect
 Mikey Bear used to require sedation before blood draws, but I showed his amazing humans how to hold his back leg for a blood draw and wet the vein while giving him treats to get him used to the feeling. They worked on this for a month, and when they came back, the blood draw was a snap. I discovered they had added another step to the homework and were poking the vein with a toothpick at home.
Mikey Bear used to require sedation before blood draws, but I showed his amazing humans how to hold his back leg for a blood draw and wet the vein while giving him treats to get him used to the feeling. They worked on this for a month, and when they came back, the blood draw was a snap. I discovered they had added another step to the homework and were poking the vein with a toothpick at home.
Jessica Jaffe, CVT, VCA Wakefield Animal Hospital, Wakefield, Massachusetts
Thinking Outside the Office
I was on primary care rotations at University of Wisconsin Teaching Hospital, and my first case of the day was a 150-pound Great Dane who had a history of being nervous during veterinary visits and in the presence of strangers. When I was notified that he and the owner had arrived, she went to the waiting room but was told that they were outside in the car. Even with sedation prior to the visit, he was too afraid to come out of the car. After speaking with the owner and assessing the situation, I decided that additional sedation and performing the exam in the car would spare him an immense amount of stress. We moved slowly, made intentional actions, and kept him comfortable. The smooth experience left the owner grateful. I firmly believe we took the pet out of petrified.
Bianca Ferlisi, veterinary student, University of Wisconsin School of Veterinary Medicine
From Terror to Trust
 When I worked at a veterinary emergency clinic, one of the dogs in the hospital was so fearful that he would begin to thrash and hit his head in the ground if anyone touched his leash. I sat in front of his cage with my back to him so he could become accustomed to my scent. Then I started placing treats in his cage and turning my back again. Eventually, I opened the door and put a leash on him and sat next to the door. When he came out of the cage on his own, I was able to walk him with no tension on the leash. Gaining an animal’s trust is a beautiful thing.
When I worked at a veterinary emergency clinic, one of the dogs in the hospital was so fearful that he would begin to thrash and hit his head in the ground if anyone touched his leash. I sat in front of his cage with my back to him so he could become accustomed to my scent. Then I started placing treats in his cage and turning my back again. Eventually, I opened the door and put a leash on him and sat next to the door. When he came out of the cage on his own, I was able to walk him with no tension on the leash. Gaining an animal’s trust is a beautiful thing.
Shelby L. Dan, veterinary assistant, Downtown Animal Hospital, Toronto, Ontario, Canada








